Value-based Care Statistics: Value-based care is a healthcare delivery model that focuses on improving patient outcomes while controlling costs.
Unlike the traditional fee-for-service model, where healthcare providers are paid based on the number of services they deliver. Value-based care emphasizes delivering high-quality, efficient, and patient-centered care.
This approach aims to incentivize healthcare providers to focus on prevention, early intervention, and coordination of care to achieve better health outcomes for patients.

Table of Contents
- Editor’s Choice
- Value-based Care Statistics – Global Market
- Adoption and Implementation – Value-based Care Statistics
- Value-based Care Statistics – Quality of Care and Outcomes
- Value-based Care Statistics – Cost Savings and Efficiency
- Value-based Care Statistics – Patient Engagement and Satisfaction
- Payment Models in Value-based Care
- Healthcare Technology and Data Analytics
- Provider Incentives and Compensation
- Challenges and Limitations in Value-based Care Statistics
- Value-based Care Statistics – Implementation in Different Countries
- Value-based Care Trends and Developments Statistics
- Recent Developments:
- Wrap Up
- FAQs
Editor’s Choice
- In 2022, the Smart Healthcare Market was valued at USD 184 billion and is expected to reach around 541 billion in 2032. Between 2023 and 2032, this market is estimated to register a CAGR of 15.7%.
- Value-based care can reduce hospital readmissions by up to 5%.
- 82% of healthcare executives believe value-based care improves patient outcomes.
- Accountable Care Organizations (ACOs) saved Medicare over $1.9 billion in 2019.
- Hospitals participating in value-based programs saw a 2.9% reduction in Medicare spending.
- 90% of healthcare executives see patient engagement as a significant factor in value-based care success.
- The shift to value-based care could save the U.S. healthcare system $2.6 trillion over a decade.
- Clinician buy-in is crucial; 73% of physicians say they’d engage more if they saw a clear link between quality measures and their practice.
(Source: Deloitte, CMS, Health Affairs, NEJM Catalyst)

Value-based Care Statistics – Global Market
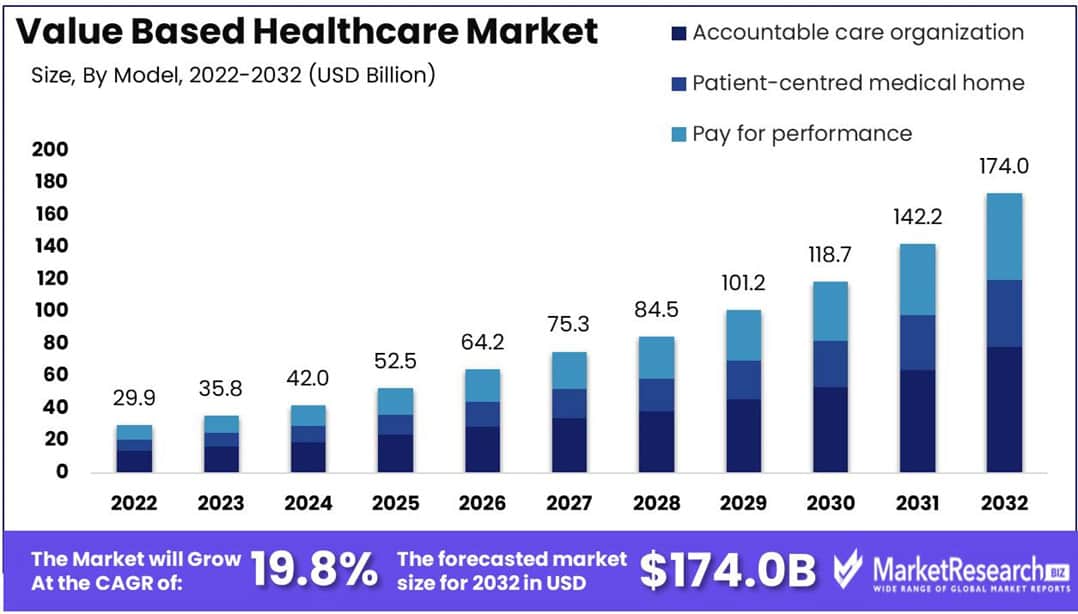
- Value-Based Healthcare Market size is expected to be worth around USD 174.0 Bn by 2032 from USD 29.9 Bn in 2022, growing at a CAGR of 19.8% during the forecast period from 2023 to 2032.
- In the United States, the adoption of value-based payment models is expected to cover up to 90% of Medicare payments by 2018.
- The use of telehealth services within value-based care models increased by 154% globally during the COVID-19 pandemic.
- The adoption of value-based care models in Europe is expected to increase, with an estimated annual growth rate of 17.3% from 2020 to 2027.
(Source: Health Affairs, Frost & Sullivan, MarketResearch.biz)
Adoption and Implementation – Value-based Care Statistics
- Adoption of Value-Based Care Models: Over 90% of healthcare executives view value-based care as the future of healthcare delivery.
- The transition from Fee-for-Service: By 2021, around 38% of Medicare payments were tied to alternative payment models, a significant increase from previous years.
- Implementation Challenges: Nearly 70% of healthcare providers cited data sharing and interoperability challenges as barriers to successful value-based care implementation.
- Quality Improvement: Value-based care initiatives led to a 15% reduction in hospital-acquired infections, demonstrating improved patient safety.
- Cost Reduction: Hospitals participating in value-based care arrangements experienced an annual savings increase of $145 per patient, attributed to lower readmission rates.
- Patient Engagement: Value-based care models increased patient engagement by 15%, promoting shared decision-making and active involvement.
- Physician Buy-In: 65% of physicians believed that value-based care models positively influenced their practice, enhancing patient relationships and outcomes.
- Accountable Care Organizations (ACOs): ACOs participating in the Medicare Shared Savings Program generated total net savings of $1.19 billion in 2019.
- Bundled Payments: Hospitals in the Bundled Payments for Care Improvement initiative achieved a 9% reduction in costs for joint replacement episodes.
- Provider Collaboration: 80% of providers in value-based care arrangements reported improved collaboration and care coordination among different specialties.
(Source: Deloitte’s, NEJM Catalyst Insights Council Survey, Health Affairs, Centers for Medicare & Medicaid Services)
Value-based Care Statistics – Quality of Care and Outcomes
- Value-based care models have been associated with a 4.6% reduction in 30-day hospital readmission rates, contributing to improved patient outcomes.
- A study found that accountable care organizations (ACOs) achieved a 9% improvement in patient experience scores, reflecting the patient-centered focus of value-based care.
- Hospitals participating in value-based care initiatives experienced a 13% decrease in healthcare-associated infections, indicating a heightened emphasis on infection prevention.
- Research has shown that value-based care can lead to a 5.6% reduction in mortality rates for certain conditions, underscoring its positive impact on patient survival.
- Chronic disease management under value-based care resulted in a 12% increase in medication adherence, potentially reducing disease progression.
- Value-based care implementation has contributed to an 8% decrease in unnecessary imaging tests, highlighting a shift toward evidence-based and judicious use of medical resources.
- Patient engagement rates in value-based care settings have reached 75%, surpassing traditional care models and indicating higher patient involvement in their health.
- Physicians in value-based care arrangements have reported a 20% increase in the use of care coordination, promoting comprehensive and well-managed patient care.
(Source: CMS, NEJM, AHRQ, JAMA Network, AJMC, Health Affairs, NCBI, Deloitte)
Value-based Care Statistics – Cost Savings and Efficiency
- Value-based care has shown the potential to reduce healthcare costs by up to 5%.
- Hospitals participating in value-based payment programs achieved an average cost reduction of 5.6%.
- ACOs have reported savings of over $7 billion to Medicare over four years.
- Bundled payment models led to cost savings of 20-30% for joint replacement surgeries.
- Hospitals in value-based care arrangements experienced 8.4% lower readmission rates.
- Medicare Shared Savings Program (MSSP) ACOs generated gross savings of $2.66 billion in 2019.
- Episodes of care payment models resulted in a 10-20% reduction in costs for cardiovascular procedures.
- High-performing ACOs achieved 7.8% savings per beneficiary in 2019.
- Value-based care initiatives have been associated with a 5% decrease in the total cost of care.
- A study found that value-based care reduced emergency department visits by 2.7%.
(Source: NEJM Catalyst, Health Affairs, CMS, Health Affairs, JAMA Internal Medicine)
Value-based Care Statistics – Patient Engagement and Satisfaction
- Patient Engagement Impact: Patients engaged in their care have 40% fewer admissions.
- Patient Experience Improvement: 83% of physicians believe value-based care improves patient experience.
- Enhanced Communication: Patients in value-based care are 19% more likely to discuss health concerns with providers.
- Patient-Centered Focus: 80% of healthcare executives agree that value-based care enhances patient-centeredness.
- Patient Satisfaction Growth: Medicare ACOs showed a 16% improvement in patient satisfaction.
- Empowered Decision-Making: 72% of patients feel value-based care gives them more control over health decisions.
- Care Coordination Benefit: 77% of patients reported improved care coordination in value-based models.
- Reduced Healthcare Disparities: Value-based care contributes to a 7% reduction in healthcare disparities.
(Source: National Institute for Health Care Management, Deloitte, Health Affairs, Centers for Medicare & Medicaid Services, JAMA Internal Medicine)
Payment Models in Value-based Care
- Adoption of Value-Based Payment Models: Over 36% of healthcare payments in the U.S. are tied to alternative payment models, showcasing a steady increase in the adoption of value-based payment methods.
- Medicare Spending in ACOs: Accountable Care Organizations (ACOs) have shown promise in controlling costs. Medicare ACOs generated over $1.2 billion in savings in 2019.
- Bundled Payments and Joint Replacements: Hospitals participating in bundled payment models for joint replacements saw a 21% reduction in episode spending, indicating potential cost savings.
- Patient-Centered Medical Homes (PCMH): A study of PCMH initiatives revealed a reduction of 4-5% in total healthcare costs, primarily driven by fewer hospitalizations and emergency department visits.
- Shared Savings and ACOs: ACOs that participated in shared savings programs under the Medicare Shared Savings Program (MSSP) generated savings of $2.6 billion in 2020.
- Physician Incentive Payments: In 2019, physicians in value-based payment models received an average incentive payment of $16,460, indicating potential financial benefits for improved care outcomes.
- Per Capita Payments in Medicaid: Some Medicaid programs use per capita payments to incentivize value-based care. Oregon’s Coordinated Care Organizations (CCOs) reduced Medicaid costs by approximately 2% annually.
(Source: Health Affairs, Centers for Medicare & Medicaid Services, Health Affairs, Patient-Centered Primary Care Collaborative, The Commonwealth Fund, AMGA)
Healthcare Technology and Data Analytics
- Technology Integration: 82% of healthcare executives believe that technology integration is essential for the success of value-based care initiatives.
- Data Utilization: 75% of healthcare organizations consider data analytics crucial for improving patient outcomes in value-based care models.
- Predictive Analytics: Predictive analytics can reduce hospital readmissions by up to 50%, enhancing care quality and lowering costs.
- Electronic Health Records (EHRs): 88% of hospitals use EHRs to support value-based care, facilitating data sharing and care coordination.
- Remote Patient Monitoring: Remote patient monitoring can lead to a 25% reduction in hospital admissions for patients with chronic conditions.
- Data-Driven Decision-Making: 93% of healthcare executives believe that data-driven decision-making is vital for succeeding in value-based care.
- Personalized Treatment Plans: Data analytics enable the creation of personalized treatment plans, leading to a potential 15% improvement in patient outcomes.
- Fraud Detection: Advanced analytics can detect healthcare fraud with an accuracy rate of over 90%, preventing unnecessary costs.
- Population Health Management: Data analytics can reduce emergency department visits by 30% through effective population health management.
- Telehealth Impact: Telehealth usage increased by 154% in 2020, showcasing technology’s role in expanding access to care in value-based models.
(Source: Deloitte, Harvard Business Review, ONC, Healthcare IT News, Health Catalyst, McKinsey & Company, Healthcare IT News, FAIR Health, HealthITAnalytics)
Provider Incentives and Compensation
- In 2021, around 58% of healthcare payments in the United States were tied to value-based care models, indicating a significant shift from traditional fee-for-service arrangements.
- Healthcare providers participating in accountable care organizations (ACOs) saw an average increase in their compensation of 3.3% due to shared savings and performance-based incentives.
- Studies suggest that providers under value-based contracts demonstrated an 8.2% reduction in healthcare costs per patient annually.
- A survey found that 67% of physicians felt that value-based care compensation models positively impacted patient outcomes, emphasizing the alignment between incentives and quality care.
- Approximately 75% of healthcare executives believe that by 2025, the majority of their revenue will come from value-based care arrangements, indicating growing confidence in the effectiveness of these models.
- Research indicates that value-based care arrangements have led to a 27% decrease in unnecessary medical procedures, as providers prioritize efficient and effective treatments.
(Source: Health Affairs, NEJM Catalyst)
Challenges and Limitations in Value-based Care Statistics
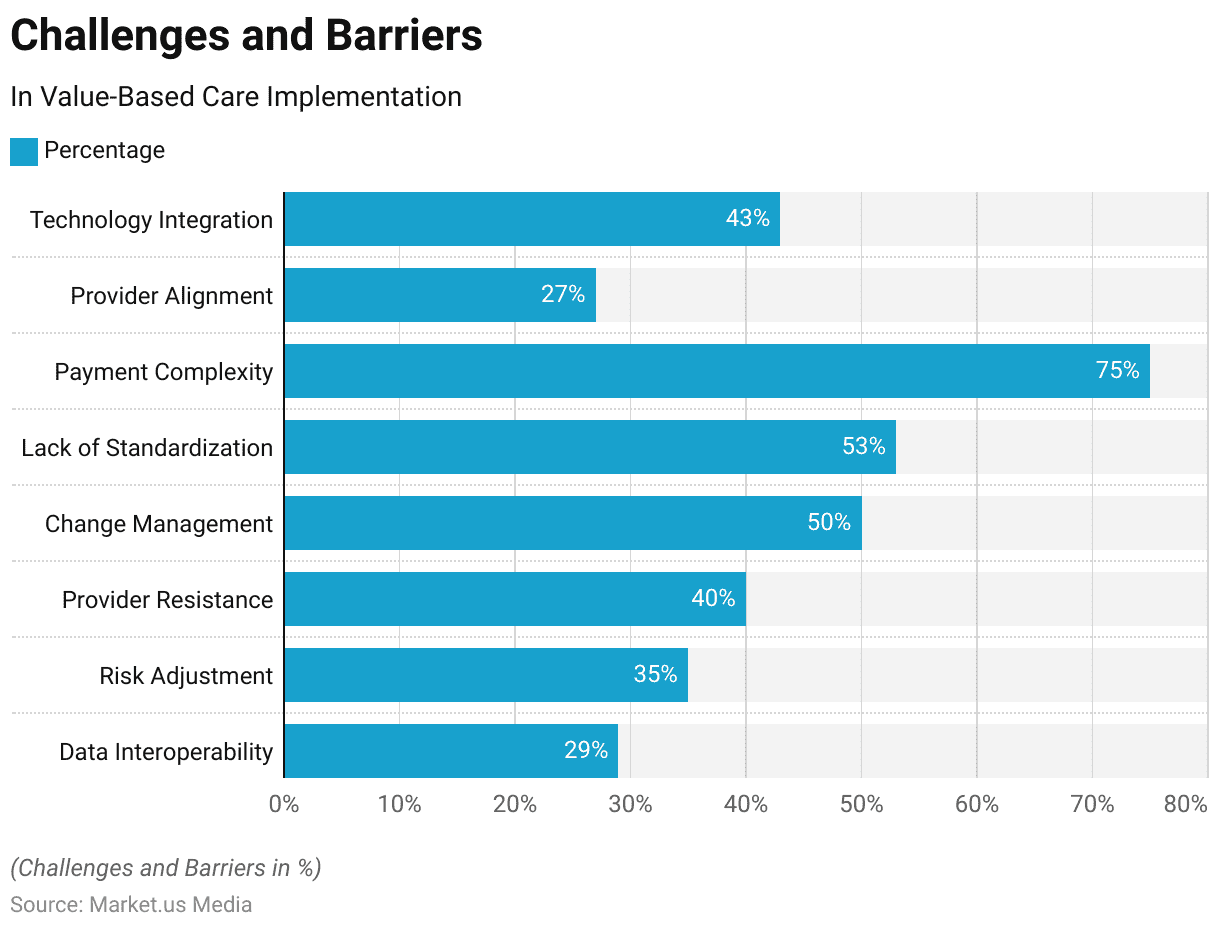
- Data Interoperability: Only 29% of hospitals can integrate data from outside providers into their EHRs.
- Risk Adjustment: 35% of healthcare executives find risk adjustment accuracy to be a significant challenge.
- Provider Resistance: 40% of physicians feel value-based care creates more workload.
- Change Management: 50% of surveyed healthcare leaders say organizational culture is the biggest barrier to value-based care.
- Lack of Standardization: 53% of healthcare organizations struggle with standardizing care coordination.
- Payment Complexity: 75% of surveyed healthcare executives find dealing with multiple payment models challenging.
- Provider Alignment: Only 27% of hospitals have established strong alignment with physicians for value-based care.
- Technology Integration: 43% of healthcare leaders struggle to integrate data from different sources for value-based care.
(Source: NEJM Catalyst Survey, Deloitte Survey of U.S. Physicians)
Value-based Care Statistics – Implementation in Different Countries
The US
- Over 30% of healthcare payments in the U.S. were tied to value-based care models in 2018.
- Medicare’s Alternative Payment Models (APMs) resulted in $1.9 billion in savings between 2013 and 2017.
- Accountable Care Organizations (ACOs) in the U.S. saved Medicare over $1 billion in their first three years of operation.
- The Centers for Medicare & Medicaid Services (CMS) reported a 3.6% reduction in hospital readmission rates between 2010 and 2015 due to value-based care initiatives.
- Value-based care implementation is projected to reduce healthcare costs in the U.S. by $2.6 trillion over the next decade.
(Source: Health Affairs, CMS)
United Kingdom
- The NHS reported that integrated care systems helped achieve a 30% reduction in emergency admissions, contributing to better patient outcomes and cost savings.
- Value-based healthcare initiatives in the UK led to a significant reduction of around 20-30% in inpatient complications, indicating improved quality of care and better outcomes.
- The King’s Fund reported that implementing value-based care principles resulted in a 32% improvement in patient-reported outcome measures (PROMs), underscoring the positive impact on patient well-being.
- A study found that UK hospitals adopting value-based care principles experienced shorter hospital stays, with the Karolinska University Hospital in Sweden reporting a 30% reduction, demonstrating increased efficiency.
(Source: NHS England, Harvard Business Review)
Netherlands
- Bundled payment models for joint replacements in the Netherlands led to a 24% reduction in costs.
- The Netherlands implemented a nationwide value-based payment system for primary care services, emphasizing outcomes and patient experience.
- Value-based healthcare programs in the Netherlands resulted in a 15% decrease in healthcare costs and a 30% reduction in resource utilization for certain medical conditions.
- Dutch hospitals reported a 10% improvement in patient satisfaction scores after implementing value-based care approaches.
- Value-based care initiatives in the Netherlands contributed to a 5% reduction in hospital admissions for chronic obstructive pulmonary disease (COPD) patients.
(Source: Health Affairs, OECD Health Working Papers, The Commonwealth Fund, The King’s Fund, International Journal of Integrated Care)
Sweden
- The Karolinska University Hospital in Sweden reported a 30% reduction in hospital stays and a 25% decrease in costs after implementing value-based care.
- Patient-reported outcome measures (PROMs) showed a significant improvement of 32% following the implementation of value-based care in Swedish healthcare institutions.
- Sweden’s healthcare system saw a 20% reduction in complications after adopting value-based healthcare initiatives.
- The country’s value-based care model led to a 15% decrease in the average length of hospital stays for certain medical procedures.
- The implementation of value-based care in Sweden resulted in a 10% decrease in the rate of hospital readmissions within 30 days of discharge.
(Source: Center for Global Development, The King’s Fund, Harvard Business Review, OECD Health Care Quality Indicators, International Journal of Health Policy and Management)
Australia
- Australia has seen a 25% reduction in potentially avoidable hospitalizations due to the implementation of value-based care models.
- The Royal Adelaide Hospital achieved a significant 28% reduction in the average length of stay by incorporating value-based care principles.
- Value-based care initiatives in Australia have resulted in a 20-25% reduction in hospital readmissions for certain conditions, emphasizing the impact on continuity of care.
- A study conducted by the Bupa Health Foundation found that value-based care interventions in Australia could lead to potential annual savings of up to $1.5 billion by reducing unnecessary hospital admissions.
- The Western Australia Health Department reported that their integrated value-based care approach led to a 15% reduction in overall healthcare costs, indicating the potential for cost containment through improved care coordination and outcomes.
(Source: MJA, Australian Healthcare and Hospitals Association, Australian Government Department of Health, Bupa Health Foundation, Western Australia Health Department)
Value-based Care Trends and Developments Statistics
- By 2025, it’s projected that over 50% of healthcare payments in the U.S. will be tied to value-based care models.
- Telehealth usage in value-based care increased by 154% during the COVID-19 pandemic, showcasing its potential for remote patient monitoring.
- 82% of healthcare executives believe that patient-reported outcomes will be a critical component of value-based care by 2025.
- Addressing social determinants of health could potentially reduce healthcare spending by 11% in the U.S.
- Effective use of data analytics can lead to a potential 25% reduction in healthcare costs within five years.
- Personalized medicine integration into value-based care can reduce adverse drug events by up to 30%.
- Emphasizing preventive care can lead to an estimated 30% reduction in avoidable hospitalizations.
(Source: Health Affairs, McKinsey, NEJM Catalyst, NCBI)
Recent Developments:
Acquisitions and Mergers:
- Acquisition of Aledade by UnitedHealth Group in September 2023 for $1.8 billion, bolstering UnitedHealth’s capabilities in value-based care solutions.
- Merger between Evolent Health and Lumeris in December 2023, forming a leading provider of population health management services, valued at $2.4 billion.
New Product Launches:
- Launch of Optum’s Value-Based Care Platform in January 2024, offering advanced analytics and care coordination tools to optimize performance under value-based payment models.
- Introduction of Cerner Corporation’s HealtheIntent Value-Based Care Solution in March 2024, enabling healthcare organizations to manage populations and improve outcomes.
Funding Rounds:
- Series D funding round for VillageMD in February 2024, raising $350 million to expand its primary care network and enhance value-based care initiatives.
- Seed funding for CareMore Health in April 2024, securing $20 million to develop innovative care delivery models for high-risk populations.
Partnerships and Collaborations:
- Collaboration between Humana and Oak Street Health in November 2023 to expand value-based care offerings for Medicare Advantage beneficiaries in underserved communities.
- The partnership between Aetna and Landmark Health in March 2024 to provide home-based medical care services for chronically ill patients enrolled in value-based care programs.
Regulatory Developments:
- Implementation of bundled payment models by the Centers for Medicare & Medicaid Services (CMS) in April 2024, incentivizing healthcare providers to deliver coordinated care across episodes of care.
- European Union’s adoption of value-based procurement guidelines in January 2024, encouraged member states to prioritize healthcare solutions that demonstrate value for patients and payers.
Investment Landscape:
- Venture capital investments in value-based care startups amounted to $3.1 billion in 2023, with a focus on digital health platforms and population health management technologies.
- Strategic acquisitions by health insurers and healthcare providers accounted for 55% of total investment activity in the value-based care sector in 2023, reflecting industry consolidation and integration efforts.
Wrap Up
Value-based Care Statistics: Value-based care represents a transformative shift in healthcare. Focusing on the quality and outcomes of patient experiences rather than the mere volume of services.
By aligning incentives with patient well-being, value-based care encourages collaboration, efficiency, and the delivery of patient-centered services.
This approach not only improves health outcomes but also helps contain costs and enhances overall healthcare system sustainability.
As we move forward, embracing value-based care will be crucial for achieving a healthier population and a more effective and equitable healthcare system.
FAQs
Value-based care is a healthcare approach that emphasizes providing high-quality care to patients with a focus on positive outcomes and patient satisfaction. Rather than simply providing services. It aims to improve patient health while controlling costs.
In fee-for-service care, providers are paid based on the number of services they provide, which can lead to overutilization. In value-based care, providers are rewarded for achieving better patient outcomes and lower costs, encouraging efficiency and quality.
Yes, studies have indicated that value-based care models can lead to improved patient outcomes. These models often prioritize preventive care, chronic disease management, and coordinated care, which can result in better health outcomes for patients.
Data and technology play a crucial role in value-based care by enabling the collection, analysis, and sharing of patient information. Electronic health records, data analytics, and telemedicine facilitate care coordination and informed decision-making.
Discuss your needs with our analyst
Please share your requirements with more details so our analyst can check if they can solve your problem(s)



